Finding out you have an ovarian cyst can mess with your head a little, especially if you’re trying to get pregnant or you plan to soon. One of the first questions people ask is: can ovarian cyst cause infertility?
Sometimes it can. Many times it does not. The tricky part is that “ovarian cyst” is a broad label. Some cysts are basically part of a normal cycle and disappear on their own. Others are linked to hormone conditions or endometriosis, and those can make it harder to conceive.
This guide breaks it down in a simple, practical way: what cysts are, how they can affect ovulation, what symptoms to look for, and what ovarian cyst treatment usually looks like when fertility is part of the conversation.
What Are Ovarian Cysts?
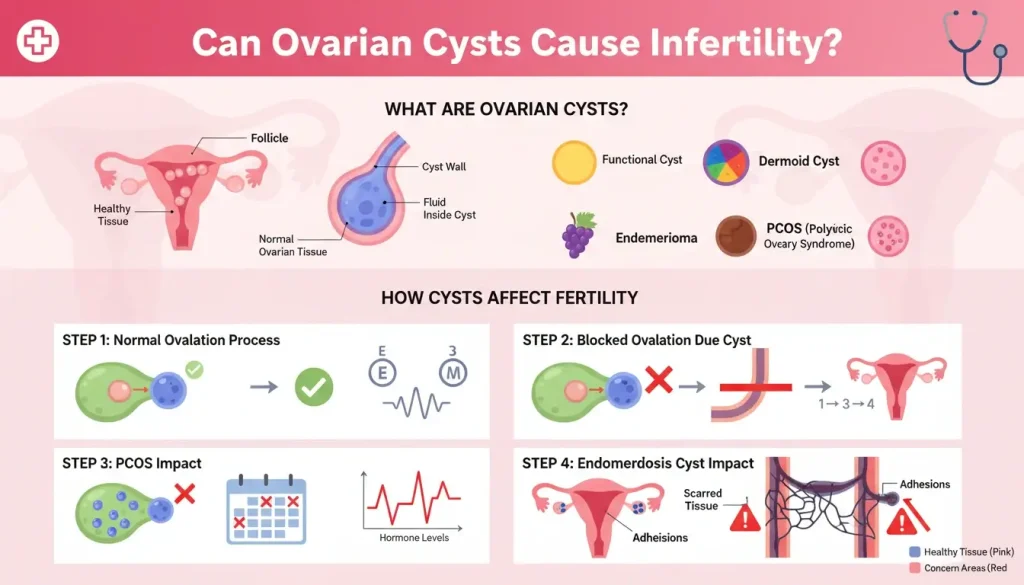
An ovarian cyst is a fluid-filled sac (or sometimes a more solid growth) on or inside an ovary. Ovaries are active organs. They grow follicles, release eggs, and respond to shifting hormones every month. Because of that, small cyst-like structures can show up even when everything is working normally.
A few points that help put things in perspective:
- Many ovarian cysts are “functional.” These are related to ovulation and often go away within a cycle or two.
- Some cysts are linked to a condition, like PCOS or endometriosis, and those may need more attention.
- Size and appearance matter. A simple, small cyst on ultrasound is usually less concerning than a large or complex one.
You might find out about a cyst during an ultrasound for irregular periods, pelvic pain, fertility testing, or even a routine check for something else.
Common types include:
- Follicular cysts: A follicle grows, but the egg doesn’t release.
- Corpus luteum cysts: After ovulation, the follicle changes into a structure that supports early pregnancy hormones. Sometimes it seals and fills with fluid.
- Dermoid cysts (teratomas): Usually benign, can contain different tissue types.
- Cystadenomas: Usually benign growths that can get large.
- Endometriomas: Cysts caused by endometriosis, often filled with old blood.
- PCOS-related “cysts”: These are usually many small follicles and a hormone pattern that disrupts ovulation.
Not all of these impact fertility in the same way.
Can Ovarian Cysts Cause Infertility?
Let’s answer it clearly: yes, ovarian cysts can cause infertility in some cases, but plenty of people with cysts conceive without any problem. The real issue is whether the cyst is:
- Blocking or disrupting ovulation, or
- A sign of an underlying condition that affects fertility
Cysts that usually do not cause infertility
Functional cysts often fall into this category:
- A follicular cyst might delay ovulation in that cycle.
- A corpus luteum cyst can show up after ovulation and still be part of a normal process.
These usually resolve on their own. They can be annoying and sometimes painful, but they’re not typically a long-term fertility problem.
Cysts that are more likely to affect fertility
This is where the “it depends” comes in.
- Endometriomas: These are tied to endometriosis, which is associated with inflammation, scar tissue, and sometimes blocked tubes. Even when tubes are open, endometriosis can still affect fertility in ways doctors don’t completely understand.
- PCOS-related ovarian changes: PCOS is one of the most common reasons for irregular ovulation. The “cysts” in PCOS are often immature follicles that don’t progress to ovulation regularly.
- Large cysts or complex cysts: A large cyst can interfere with normal ovarian function, cause pain during sex, or lead to complications like torsion. Sometimes the treatment (including surgery) can also affect ovarian reserve, depending on the situation.
- Infection-related cysts/abscesses: Less common, but pelvic infections can cause scarring and fertility issues.
So when someone asks about ovarian cyst and fertility, the best next question is usually: What type of cyst is it, and what does your cycle look like right now?
How Ovarian Cysts Affect Ovulation
Ovulation is the release of an egg from the ovary. It’s driven by a back-and-forth conversation between your brain (pituitary hormones like FSH and LH) and your ovaries (estrogen and progesterone).
Cysts can interfere with ovulation in a few ways:
- A functional cyst can disrupt timing. If a follicle doesn’t rupture, the egg isn’t released. Your period may come late, or your cycle may feel “off” that month.
- PCOS can lead to irregular or absent ovulation. Many people with PCOS have follicles that start developing but don’t mature consistently. That’s one reason cycles can be long, unpredictable, or skipped.
- Endometriomas can affect ovarian function. Not everyone with an endometrioma struggles with fertility, but there may be effects on egg quality, inflammation levels, or how the ovary responds to hormones.
- Large cysts can physically distort the ovary. Sometimes the issue is mechanical. The ovary isn’t functioning in its usual way because something is taking up space.
If you’re trying to conceive, it can help to track signs of ovulation (like cycle length patterns, ovulation predictor kits, basal body temperature, or cervical mucus). It’s not perfect, but it gives useful clues.
Symptoms of Ovarian Cysts
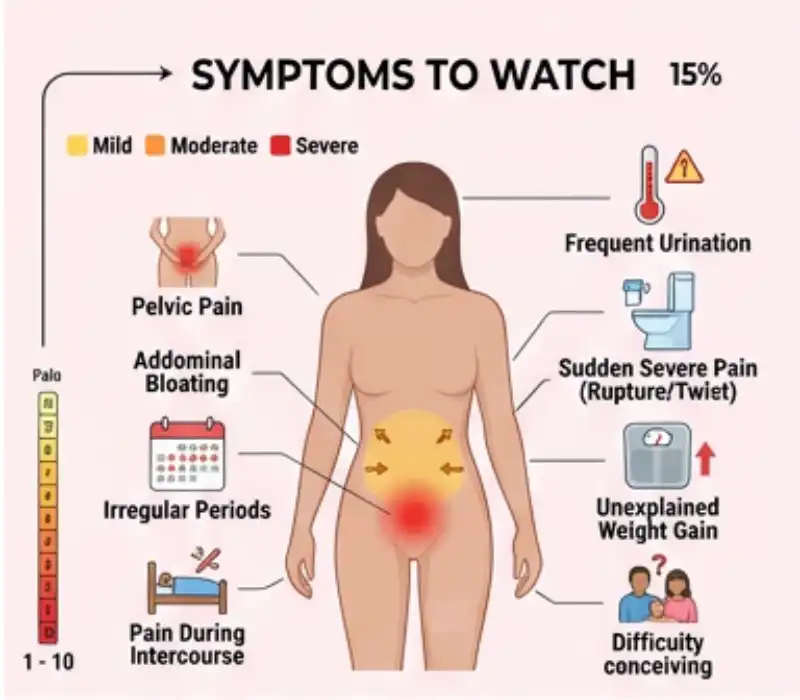
Some cysts cause no symptoms at all. When symptoms do show up, they can be vague, which is why people often brush them off for a while.
Here are common symptoms of ovarian cyst that people actually notice in day-to-day life:
- Pelvic pain on one side (dull, sharp, or throbbing)
- Bloating or a heavy feeling in the lower abdomen
- Pain that flares around ovulation or before a period
- Pain during sex, especially deeper penetration
- A feeling of pressure on the bladder, needing to pee more often
- Changes in periods (heavier, lighter, irregular, spotting)
- Lower back pain or a sense of pelvic pressure
- Pain with bowel movements (sometimes, depending on location)
Symptoms that deserve urgent care
A cyst can rupture or an ovary can twist (torsion). Those are not things to “wait out.”
Get urgent medical help if you have:
- Sudden, severe pelvic pain
- Pain with vomiting or fever
- Dizziness, fainting, or weakness
- Rapid worsening pain that doesn’t settle
Can You Get Pregnant with an Ovarian Cyst?
A common question is: can you get pregnant with ovarian cyst?
In many cases, yes.
If the cyst is functional and you’re ovulating, pregnancy can still happen. Some people even find out about a cyst early in pregnancy because the corpus luteum can look cyst-like on ultrasound.
Pregnancy can be more complicated if:
- You’re not ovulating regularly (often the case with PCOS).
- The cyst is an endometrioma and endometriosis is affecting tubes or pelvic anatomy.
- The cyst is large and causing pain or needs surgical treatment.
- You’re dealing with multiple factors at once, like thyroid issues, male factor infertility, or age-related changes.
It’s also worth saying out loud: fertility is rarely about one thing. A cyst might be part of the picture without being the whole story.
If you’re actively trying, it’s reasonable to ask your doctor:
- Am I ovulating?
- What type of cyst is this?
- Do we need to treat the cyst, the ovulation pattern, or both?
Treatment Options for Ovarian Cysts
Ovarian cyst treatment is not one-size-fits-all. It’s usually based on:
- Your symptoms (pain, bloating, cycle changes)
- The cyst type and size
- Ultrasound features (simple vs complex)
- Your age and medical history
- Whether you’re trying to conceive now
Some cysts just need monitoring. Others need a plan that includes hormones, fertility support, or surgery.
Medical Treatment Options
1) Watchful waiting (monitoring)
If a cyst looks simple and you’re not having severe symptoms, many clinicians recommend repeating an ultrasound after a set time to see if it shrinks or disappears. This is common with functional cysts.
2) Pain management
Anti-inflammatory pain relievers are often used, along with heat and rest. This doesn’t treat the cyst itself, but it can make life more manageable while the cyst resolves.
3) Hormonal contraception (when pregnancy is not the goal)
Birth control pills or other hormonal methods may reduce the chance of new functional cysts forming in some people. They’re not a fit if you’re actively trying to get pregnant.
4) Ovulation support (when irregular ovulation is the bigger issue)
If your cyst pattern is tied to irregular ovulation, your clinician may focus on helping you ovulate more reliably. This often comes up with PCOS.
These types of medications are sometimes used to support ovulation in certain cases, including ovulation support medications like clomiphene-based medicines (such as Siphene, Clofert, Clomisign). They’re not right for everyone, and they’re typically used with cycle monitoring so timing and response are clear.
In some treatment plans, clinicians may also use fertility treatment options such as fertility support injections like HCG (Ovidac, Hucog) to support ovulation timing in specific situations.
And when progesterone levels need support after ovulation (for example, in certain luteal phase concerns), progesterone support like Susten or Duphaston may be discussed. This depends on your history and test results.
5) Surgery
Surgery might be recommended when a cyst is:
- Large
- Persisting over time
- Causing significant pain
- Complex-looking on ultrasound
- Suspicious for torsion risk
- An endometrioma that is affecting function or causing symptoms
Common procedures include cyst removal (cystectomy). If fertility is a priority, most surgeons aim to preserve as much healthy ovarian tissue as possible. Still, there can be trade-offs, especially with endometriomas, because removing the cyst wall can sometimes remove normal tissue too. This is a good conversation to have before surgery, not after.
It’s always best to talk to a doctor before starting any medication.
Hormonal Balance Treatment
A lot of people hear “hormones” and assume that means a single pill fixes everything. Real life is messier.
If your clinician suspects a hormone imbalance is contributing to cyst formation or irregular cycles, they may look at things like:
- Thyroid function
- Prolactin
- PCOS-related hormone patterns (androgens, insulin resistance)
- Signs of estrogen dominance or low progesterone patterns (not always simple to prove)
In some situations, hormonal therapy options may be considered to support estrogen or progesterone balance, especially when the goal is cycle regulation rather than immediate conception. This might include estrogen therapies like Progynova or Premarin in specific clinical scenarios.
If you want to read more about what’s commonly used, you can browse hormonal therapy options and then discuss with your doctor what actually fits your situation. Not everyone needs hormonal treatment, and it should be individualized.
Lifestyle and Natural Support
Lifestyle changes won’t “dissolve” every cyst, and anyone promising that is oversimplifying. Still, habits can make a real difference for hormone-related patterns, especially with PCOS and irregular ovulation.
Here are supportive steps that are generally reasonable:
- Aim for steady blood sugar
Balanced meals with protein, fiber, and healthy fats can help with insulin resistance, which is common in PCOS.
- Move your body consistently
Walking, strength training, yoga, cycling. Pick something you can stick with. Consistency matters more than intensity.
- Work toward a healthy weight if needed (without crash dieting)
For some people with PCOS, even modest weight loss can improve ovulation. For others, weight isn’t the driver. If weight change becomes stressful or obsessive, it can backfire.
- Sleep and stress support
Poor sleep and chronic stress can affect hormone signals. It doesn’t mean stress “causes” cysts, but it can influence cycle regularity.
- Track your cycle
If you’re trying to conceive, tracking ovulation signs helps you and your clinician see patterns over time. It can also reduce the feeling that everything is random.
If you’re using supplements, treat them like medications. Some can affect bleeding, thyroid levels, or interact with fertility treatments. Bring a list to your appointment.
When to See a Doctor
Some people can safely monitor a cyst. Others shouldn’t wait.
Make a routine appointment if:
- Pelvic pain keeps coming back
- Your periods become irregular or significantly more painful
- You have persistent bloating or pelvic pressure
- Sex has become painful
- You’re trying to conceive and cycles are unpredictable
- You’ve been told you have a cyst and you never got a follow-up plan
Seek urgent care if:
- You have sudden, severe pelvic pain
- Pain comes with vomiting or fever
- You faint or feel very dizzy
- You suspect pregnancy and have severe one-sided pain (ectopic pregnancy needs to be ruled out)
If you’re trying to conceive and it’s taking longer than expected, cysts may be part of the workup, but they’re rarely the only focus. Many clinicians suggest:
- Under 35: consider an infertility evaluation after 12 months of trying
- 35 and older: after 6 months
- Any age: sooner if cycles are irregular, you suspect PCOS, or endometriosis symptoms are strong
FAQ
1) Can ovarian cysts cause infertility?
Yes, they can, depending on the type. Functional cysts usually do not cause long-term infertility. Cysts linked to PCOS or endometriosis can affect fertility more often because those conditions can disrupt ovulation or the reproductive environment.
2) Can ovarian cyst cause infertility even if I have regular periods?
It’s possible, but less likely. Regular periods often suggest you’re ovulating, though it’s not a guarantee. Some cyst types (like endometriomas) can affect fertility even with fairly regular cycles.
3) Can I get pregnant with ovarian cyst?
Often yes. Many people conceive with a small functional cyst. If the cyst is tied to irregular ovulation (PCOS) or endometriosis, pregnancy is still possible, but you may need more support or a clearer plan.
4) Do ovarian cysts go away on their own?
Many do, especially functional cysts. They often resolve within one to three cycles. Cysts that persist, grow, or look complex on ultrasound need follow-up.
5) What are the most common symptoms of ovarian cyst?
Many people have no symptoms. When symptoms happen, they often include one-sided pelvic pain, bloating or pressure, pain during sex, and changes in periods.
6) When should I worry about ovarian cyst?
If you have sudden severe pain, vomiting, fever, fainting, or rapidly worsening symptoms, treat it as urgent. For non-urgent situations, follow up if the cyst is large, persistent, or causing ongoing pain or cycle disruption.
Final Thoughts
So, can ovarian cyst cause infertility? Sometimes, yes. But a cyst diagnosis isn’t automatically a fertility sentence. A lot of cysts are temporary, and even when fertility is affected, there are usually several paths forward.
If you’re trying to conceive, the most helpful next steps are figuring out what type of cyst you have, whether you’re ovulating, and whether there’s an underlying condition like PCOS or endometriosis driving the pattern. From there, treatment can be as simple as monitoring, or it might include targeted hormone support or fertility care.
And if you take one thing from all of this, make it this: it’s always best to talk to a doctor before starting any medication.